I have been thinking a great deal lately about the meaning of a “good death,” and how that relates to care work. I mull these topics not because I’m inherently morbid (although that may also be true), but because I study families caring for cancer patients at home and in the hospital. Some of the patients I know die; how they die should matter as much in assessing their quality of care as how they survived.
By most measures, patients and families report higher levels of satisfaction with end of life care in hospice or a palliative care unit than in a nursing home or ICU. 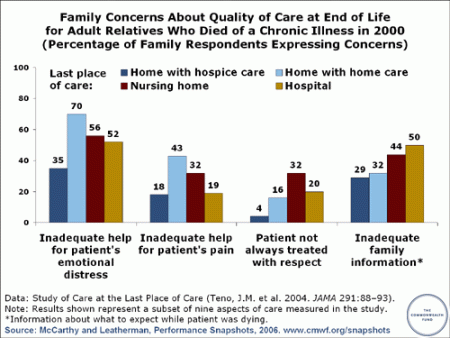 Although cancer patients are the largest subset of hospice patients, making up 46% of total admissions, only 38% of cancer patients die at home. Seventy percent of Americans surveyed indicate that they prefer to die at home; yet seventy-five percent die in an institution. Those who do receive hospice care receive less time in hospice than they need. This figure varies regionally, and may be one of the few areas of medical care in which reduced cost coincides with increased quality of care.
Although cancer patients are the largest subset of hospice patients, making up 46% of total admissions, only 38% of cancer patients die at home. Seventy percent of Americans surveyed indicate that they prefer to die at home; yet seventy-five percent die in an institution. Those who do receive hospice care receive less time in hospice than they need. This figure varies regionally, and may be one of the few areas of medical care in which reduced cost coincides with increased quality of care.
In my work with cancer patients and their families, I have attended numerous clinic visits where physicians have had the opportunity to talk about death. In most cases, they avoid the topic until death is imminent, which is usually after the patient has suffered considerable pain and before they have had the time to take in the news. Recently, I sat in on several meetings with a patient, let’s call him Steve, 59, and his wife and children as they struggled to cope with the implications of his failed bone marrow transplant. The only indication they were given by his physician came in the form of phrases like, “these are not the kids of test results we like to see.” And “you should try to maximize the good days.”
As each second- and third-line treatment failed, I watched as Steve and his family groped in the dark for answers – was he dying? Was the hoped-for miracle still out there? Ultimately, when Steve turned the final corner, was about to die, he was unable to hear his doctor tell him that he needed to come inpatient immediately for comfort care. He told his wife that he “wasn’t done fighting.” I would suggest that he hadn’t had time to take in the fact that the battle for cure had already been lost, and that a new, equally important, set of decisions about how and where he wanted to die lay before him. He died that night after a severe pain episode, in the ambulance that was rushing him to the hospital.
Oncologists are notoriously inept at talking about death, a problem I witnessed frequently in my time with dying patients. The problem is significant enough that the prestigious Hutchinson Cancer Center in Seattle has begun a foundation-funded program to teach Oncology Fellows how to address bad news. The oncology staff I have worked with describe these dilemmas with self-deprecating humor: doctors who can’t use the “d” word “circle the train,” those overly-prone to dire prognoses are “hanging crepe.” Prognosis is, of course, as much art as science, so it is not surprising that doctor’s often get it wrong. Numerous subtle conversational cues can also help or hinder the communication of news.
In my observations, however, I have noted something more fundamental in physician’s approaches to talking about death. It may be only be possible to talk about death in one of two modes. Accepting the need to talk about dying is accepting the need to address the deepest human fears and being willing to open a door to the most profound human experience. This may range from the minutiae to the metaphysical. There is no way to talk about it halfway. It may be that the options are limited to doctors who, when invited, talk about death and dying “all the way,” and those evade and avoid.
In a recent patient conference, I sat in a chemotherapy room with Alice, age 54, her husband and their two twenty-something children. She also had experienced a recurrence of Leukemia after transplant and had tried numerous experimental therapies that failed to achieve remission.
Her physician, Dr. Marshall, invited a frank exchange by explaining that he didn’t see any benefit in pursuing further aggressive chemotherapy any further, saying “we’ve been through all the buckets of chemo we can come up with, and at this point we can create lots of misery without any good value for it.” He went on to suggest a low-dose approach that might keep her disease in check for a time. After he explained the therapy, he asked if any of the family had any questions. Alice’s daughter took the conversation further, asking, “How does a person die of Leukemia?” Alice’s physician paused, looked at Alice and asked, “Do you mind if I talk about this in general….?” Alice said, “Yes, that’s why I brought them here.” This in itself is notable, in that doctors generally take their cues from patients when deciding how frank to be in end of life conversations. Alice had already reached out to a local hospice, and although she was still receiving chemotherapy to prolong her life, she was willing to talk about dying.
In the discussion that followed, Dr. Marshall outlined each possible trajectory towards death in gentle detail, in each case outlining the principles of maximizing good days and providing for comfort on bad days and the treatment plan that would be consistent with that approach given the direction of the disease. I watched the family members in the room take in each option as the doctor outlined it, groping towards the knowledge that Alice had a limited time to live. Still, this conversation laid the foundation for them to collectively and mindfully make the tough decisions to come. Thinking back to my post-mortem interview with Steve’s family and the pain on their faces as they tried to understand where in his journey they went wrong, I was grateful that Alice and her family were beginning to see their options. When Dr. Marshall left the room, having answered all of their immediate questions, Alice looked at all of us and said, “Ok, everybody breathe.”
Next: how does insurance add to the problem?